Beyond Fluid Pressure: A New Cellular Model of Ménière’s Disease
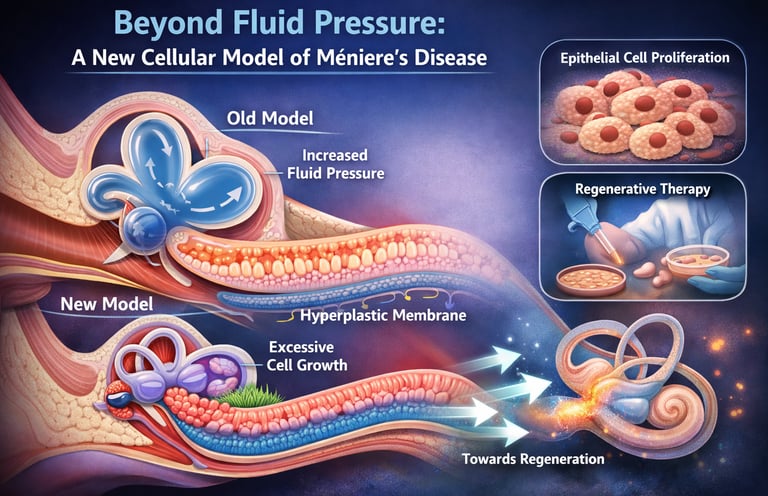
A groundbreaking study overturns the long-standing belief that Ménière’s disease is driven by inner ear fluid pressure. Instead, researchers show that excessive epithelial cell proliferation reshapes inner ear membranes, redefining endolymphatic hydrops as a hyperplastic process. This paradigm shift has major implications for how we understand disease progression—and how future therapies may target regeneration rather than pressure reduction.
12/21/2025
Rethinking Meniere’s Disease: Hyperplastic Growth, Not Fluid Pressure, Drives Inner Ear Changes
Meniere’s disease (MD) is a complex disorder of the inner ear, known for causing recurrent vertigo, fluctuating hearing, and eventually permanent sensory deficits. For decades, the prevailing explanation has been that these symptoms result from excessive inner ear fluid, known as endolymphatic hydrops (EH), which supposedly increases pressure and damages sensory cells. However, a recent study is challenging this long-held belief. By applying advanced 3D reconstructions, machine-learning-assisted histology, and immunohistochemistry to postmortem human inner ears, researchers have revealed a surprising mechanism behind EH.
Hyperplasia, Not Pressure, Underlies Endolymphatic Hydrops
Instead of finding evidence of tissue stretching or ruptures caused by fluid pressure, the study observed marked epithelial cell proliferation—a 4–7-fold increase in the number of cells in critical inner ear structures such as Reissner’s membrane and the saccular membrane. This hyperplasia was present even in early stages of EH, suggesting it occurs before advanced disease develops.
This discovery shifts the perspective from viewing EH as purely a pressure-driven phenomenon to seeing it as a cellular compensatory response. The epithelial expansion may help maintain fluid balance and support inner ear function, potentially offsetting cell loss in the endolymphatic sac, a key structure affected in MD.
Implications for Understanding and Treating Meniere’s Disease
The findings introduce a more nuanced view of EH: it may play both beneficial and detrimental roles.
While epithelial growth appears adaptive, excessive or maladaptive remodeling could contribute to disease progression.
For clinicians and researchers, this opens up new avenues for therapy:
• Promoting tissue repair to support healthy epithelial expansion
• Preventing maladaptive remodeling that could worsen symptoms
• Targeting fluid homeostasis mechanisms rather than just reducing pressure
This paradigm shift emphasizes that Meniere’s disease is not merely a fluid-overload disorder, but a condition with complex cellular responses that can be harnessed for better treatment strategies.
Why This Matters
Understanding that hyperplasia, not hydrostatic pressure, drives EH can lead to more precise interventions and a better quality of life for MD patients. Future therapies may focus on supporting the inner ear’s natural compensatory mechanisms, potentially preventing the chronic hearing and balance issues that define this disease.

Follow
Contact
info@microlab.ink
© Microlab-copyright 2026

