Biopsy Diagnosis of Celiac Disease: The Pathologist's Perspective in Light of Recent Advances
2/12/20261 min read
Introduction
Celiac disease is a chronic autoimmune disorder triggered by dietary gluten in genetically susceptible individuals. It primarily affects the small intestine, causing immune-mediated injury to the mucosal lining. Histological examination of intestinal biopsies plays a central role in the diagnosis, grading, and management of Celiac Disease, and remains the gold standard in clinical pathology.
Histopathological Features
The characteristic histological changes seen in Celiac Disease biopsies of
the duodenum or jejunum include:
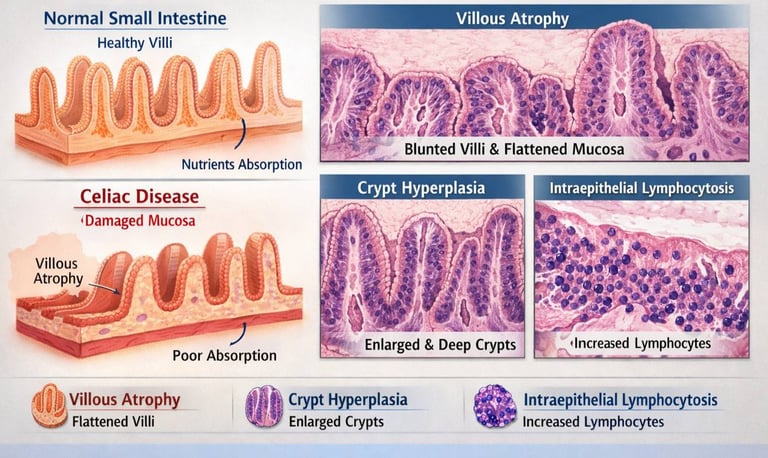
1. Villous Atrophy:
The normal finger-like villi of the small intestine are shortened or flattened, reducing the absorptive surface area.
2. Crypt Hyperplasia:
The crypts of Lieberkühn are abnormally deep and elongated, indicating increased epithelial turnover.
3. Intraepithelial Lymphocytosis:
A marked increase in the number of lymphocytes within the epithelial layer is a hallmark of the disease.
These features form the basis of histologic scoring systems like the Marsh-Oberhuber classification, which help to quantify the severity of mucosal damage from early intraepithelial lymphocytosis to total villous flattening.
Diagnostic Importance
Histological evaluation is indispensable because:
• It confirms the presence and degree of mucosal injury caused by gluten exposure.
• It helps differentiate Celiac Disease from other small bowel disorders with similar clinical symptoms but distinct histology.
• Follow-up biopsies can assess mucosal healing after initiation of a gluten-free diet or other therapeutic interventions.
Challenges and Best Practices
Despite its diagnostic value, histological evaluation has challenges, including sampling errors and interpretation variability. Recent best-practice recommendations emphasize standardized biopsy procurement, proper tissue orientation, and quantitative assessment to improve reliability.
Conclusion
Histology remains a cornerstone of Celiac Disease diagnosis and research. The distinctive pattern of villous atrophy, crypt hyperplasia, and lymphocytic infiltration provides critical evidence of mucosal injury and guides both clinical management and future studies in disease pathogenesis

Follow
Contact
info@microlab.ink
© Microlab-copyright 2026

